Cognitive Behavioural Therapy (CBT) has the strongest evidence base of all talking therapies for successful treatment of anxiety disorders and depression. It is therefore recommended as treatment of first choice by the UK’s National Institute for Health and Care Excellence (NICE) with a BABCP-accredited expert.
Cognitive-behavioural therapy (CBT) is all about the relationship between emotions, thoughts and behaviour. It focuses on helping us understand how our thinking about a situation affects the way we feel and act. It’s an active, collaborative and change-focused type of approach, and client and therapist work together to change the client’s behaviours, or their thinking patterns or, most often, both.
CBT is pragmatic and structured, and attending appointments is a starting point. To get the most out of therapy, we ask clients to put things into practice between sessions. Early on in the therapy this might be keeping a diary of thoughts, feeling and behaviours, assigned reading or listening to relevant audio. Later on in the process, we’ll be harnessing our inner scientists, and designing creative challenges that try out new ways of behaving. This might make you feel uncomfortable to begin with, but by repeating these challenges you will get used to behaving differently.
It’s important to us that the hard work you put in during sessions actually leads to changes in your life.
Depending on the issue that brings people to therapy, some see huge improvement in 6-8 sessions when there is a single focus such as sleep disturbance or phobias. More complex or longstanding issues will take a greater number of sessions, so we will have regular reviews along the way to ensure that you are finding CBT helpful.
Whether you’re experiencing anxiety or more of a depressive problem, we’ll look at the problematic patterns of thinking, feeling and behaviour in a vicious cycle. These cycles highlight the maintaining processes.
Identifying these cycles of unhelpful behaviour is key in the early stage of CBT. We need to be able to recognise patterns, so you can then intercept and change them.
Let’s look at the two most common categories of behavioural maintaining processes: safety behaviours and escape/avoidance.
Safety behaviours occur when you want to protect yourself from something you fear and are often seen in anxiety disorders. For example, if you suffer from panic disorder, examples of this type of behaviour include carrying water ‘just in case’, sitting down if your heart rate increases or taking a diazepam before going on the Tube. Here it is in a vicious cycle:
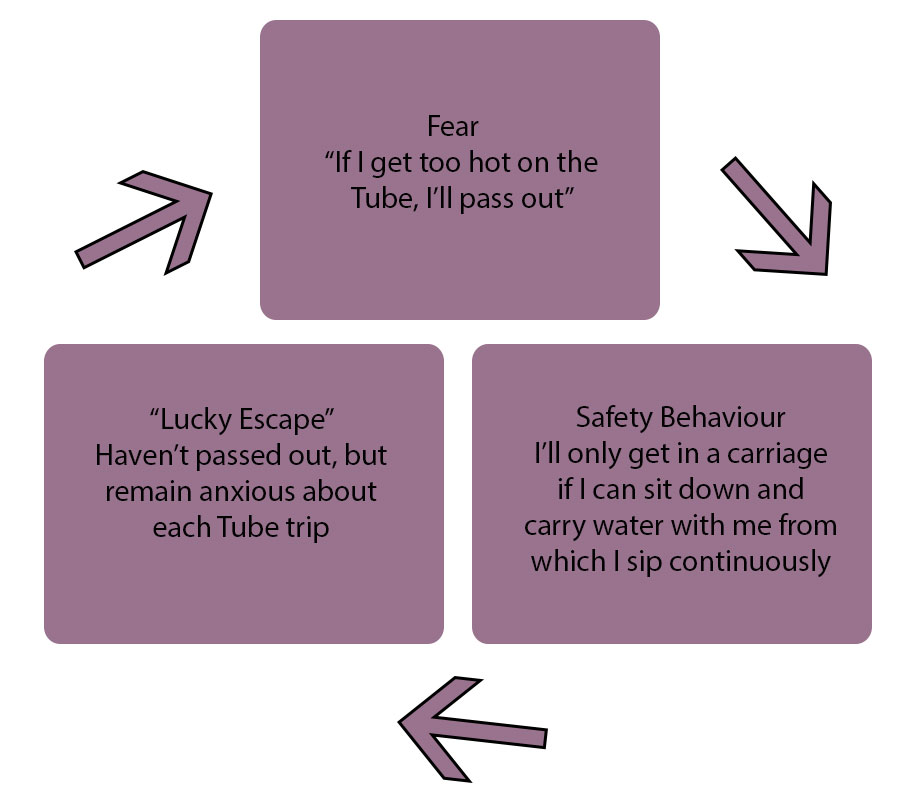
While it’s understandable to try and find strategies that help you cope with unpleasant feelings of anxiety, these behaviours can backfire as the actual problem remains unresolved. This is the case across the disorders, for example, if you’re health anxious, although you managed to feel less anxious the last time you did your daily check for new moles/lumps/changes in your body, you’re going to feel just as anxious tomorrow morning and repeat the behaviour to reduce the unpleasant feelings.
It’s very common when you’re feeling anxious to want to run away from the situation that is making you feel tense. This is why if you suffer, for example, social anxiety, you might tend to avoid social situations entirely, choosing to be on your own and withdraw. Or you may go, but avoid eye contact, stand on the edge of a group, and hope no one will talk to you. Like other safety behaviours, avoidance and escape can actually make your anxiety worse in the long run, because they undermine your confidence and prevent you from discovering if your fears are founded on reality, or are just extreme and unhelpful
Unlike more traditional forms of therapy, CBT (and all our therapists) firmly believe that you have the power to break out of this cycle, and our role is to help you discover how.
| Cookie | Duration | Description |
|---|---|---|
| __stripe_mid | 1 year | This cookie is set by Stripe payment gateway. This cookie is used to enable payment on the website without storing any payment information on a server. |
| __stripe_sid | 30 minutes | This cookie is set by Stripe payment gateway. This cookie is used to enable payment on the website without storing any payment information on a server. |
| cookielawinfo-checkbox-advertisement | 1 year | Set by the GDPR Cookie Consent plugin, this cookie is used to record the user consent for the cookies in the "Advertisement" category . |
| cookielawinfo-checkbox-analytics | 1 year | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Analytics". |
| cookielawinfo-checkbox-functional | 1 year | The cookie is set by GDPR cookie consent to record the user consent for the cookies in the category "Functional". |
| cookielawinfo-checkbox-necessary | 1 year | This cookie is set by GDPR Cookie Consent plugin. The cookies is used to store the user consent for the cookies in the category "Necessary". |
| cookielawinfo-checkbox-others | 1 year | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Other. |
| cookielawinfo-checkbox-performance | 1 year | This cookie is set by GDPR Cookie Consent plugin. The cookie is used to store the user consent for the cookies in the category "Performance". |
| elementor | never | This cookie is used by the website's WordPress theme. It allows the website owner to implement or change the website's content in real-time. |
| viewed_cookie_policy | 1 year | The cookie is set by the GDPR Cookie Consent plugin and is used to store whether or not user has consented to the use of cookies. It does not store any personal data. |
| Cookie | Duration | Description |
|---|---|---|
| _ga | 2 years | The _ga cookie, installed by Google Analytics, calculates visitor, session and campaign data and also keeps track of site usage for the site's analytics report. The cookie stores information anonymously and assigns a randomly generated number to recognize unique visitors. |
| _gat_gtag_UA_191518058_1 | 1 minute | Set by Google to distinguish users. |
| _gid | 1 day | Installed by Google Analytics, _gid cookie stores information on how visitors use a website, while also creating an analytics report of the website's performance. Some of the data that are collected include the number of visitors, their source, and the pages they visit anonymously. |